Researchers in Singapore conducted a study showing that the messenger RNA (mRNA) -based 2019 coronavirus disease (COVID-19) vaccines developed by Pfizer-BioNTech and Moderna are highly effective in protecting against symptomatic and severe illness after infection with the rapidly spreading B virus. .1.617.2 (delta) variant of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
The team conducted a retrospective multicenter cohort study of vaccinated and unvaccinated individuals who had been admitted to hospital following infection with the variant of concern B.1.617.2.
“To our knowledge, we provide the first data characterizing the impact of vaccination on virologic kinetics by the B.1.617.2 variant,” writes Barnaby Young of the National Center for Infectious Diseases in Singapore and colleagues.
The team found that people fully vaccinated with Pfizer-BioNTech’s BNT162b2 vaccine or Moderna’s mRNA-1273 product were significantly less likely to develop moderate or severe outcomes after infection with B.1.617.2 than people without vaccinated.
Vaccination was associated with fewer symptoms, lower peak biomarkers of systemic inflammation, and better clinical outcomes. It was also associated with a faster drop in viral RNA load and a robust serological response.
“Vaccination remains a key strategy for controlling the COVID-19 pandemic,” says Young and colleagues.
A pre-printed version of the research paper is available on the site medRxiv* server, while the article is subject to peer review.
Worrisome variants threaten immunization efforts
Phase 3 clinical trials of mRNA vaccines have demonstrated 92% to 95% efficacy in preventing symptomatic and severe disease after infection with SARS-CoV-2.
While the massive deployment of these vaccines has reduced infection and death rates in many countries, the emergence of variants of SARS-CoV-2 containing mutations in the viral spike protein has raised growing concerns about the disease. increased transmissibility and resistance to vaccine-induced immunity.
The spike protein is the primary structure the virus uses to infect cells and a primary target for binding and neutralizing antibodies after natural infection or vaccination.
While worrying variants such as B.1.1.7 (alpha), B.1.351 (beta), P.1 (gamma) and B.1.617.2 (delta) have all shown increased transmissibility, the B. 1.1.7 and B.1.617.2 have also been associated with an increase in the severity of illness and hospitalizations.
Following the emergence of B.1.617.2 in India, this variant quickly spread to other countries and had become the most frequently sequenced lineage worldwide by the end of June 2021.
The vaccination program in Singapore
The COVID-19 vaccination program began in Singapore on December 30e2020
July 19e, 2021, more than 6,837,000 doses of vaccine had been administered and approximately 2,792,400 people had been fully immunized.
What did the researchers do?
Young and colleagues conducted a retrospective multicenter cohort study to characterize the clinical, virological and serological characteristics of vaccinated adults with B.1.617.2 infection. The results were compared with those of unvaccinated patients who also had B.1.617.2 infection.
Participants were recruited between April 1st and June 14e, 2021, at five study sites: the National Center for Infectious Diseases, Singapore General Hospital, National University Hospital, Changi General Hospital and Sengkang Hospital.
What did the study find?
Of 218 people diagnosed with B.1.617.2 infection by polymerase chain reaction (PCR), 88 had received a vaccine.
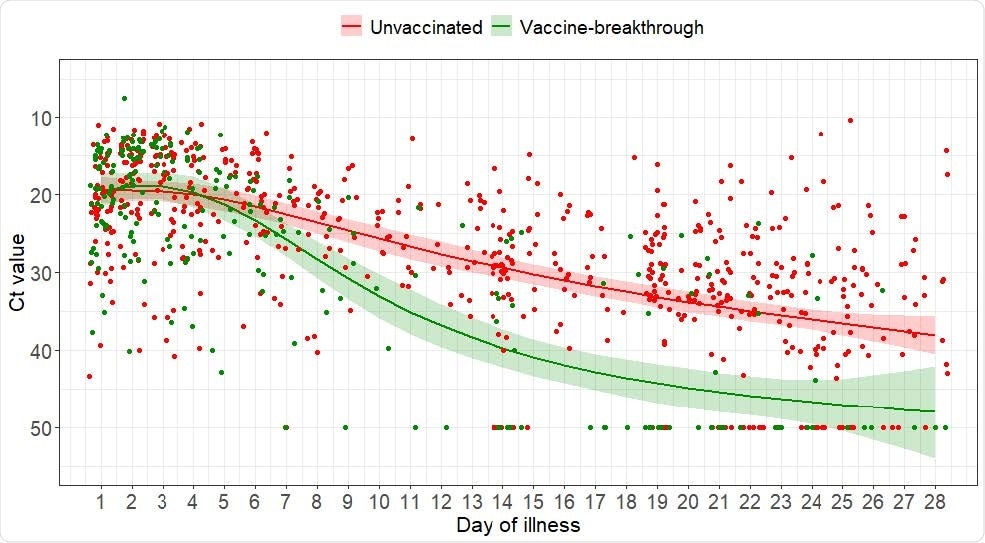
Scatter plot of Ct values and marginal effect of the day of illness of patients infected with COVID-19 B1.617.2 with 95% confidence intervals from a generalized additive mixed model with interaction term between vaccination status and the day of illness
Seventy-one people were fully vaccinated and therefore met the definition of a vaccine disruption infection. Sixty-six of these participants (93%) had received two doses of Pfizer-BioNTech BNT162b2 vaccine.
The vaccine infection cohort was significantly older than the unvaccinated cohort, with a median of 56 years (age range 39 to 64) versus 39.5 years (age range 30 to 58 ). People with a breakthrough infection were also significantly more likely to be asymptomatic (at 28.2% vs. 9.2%) and to have fewer symptoms if they were symptomatic.
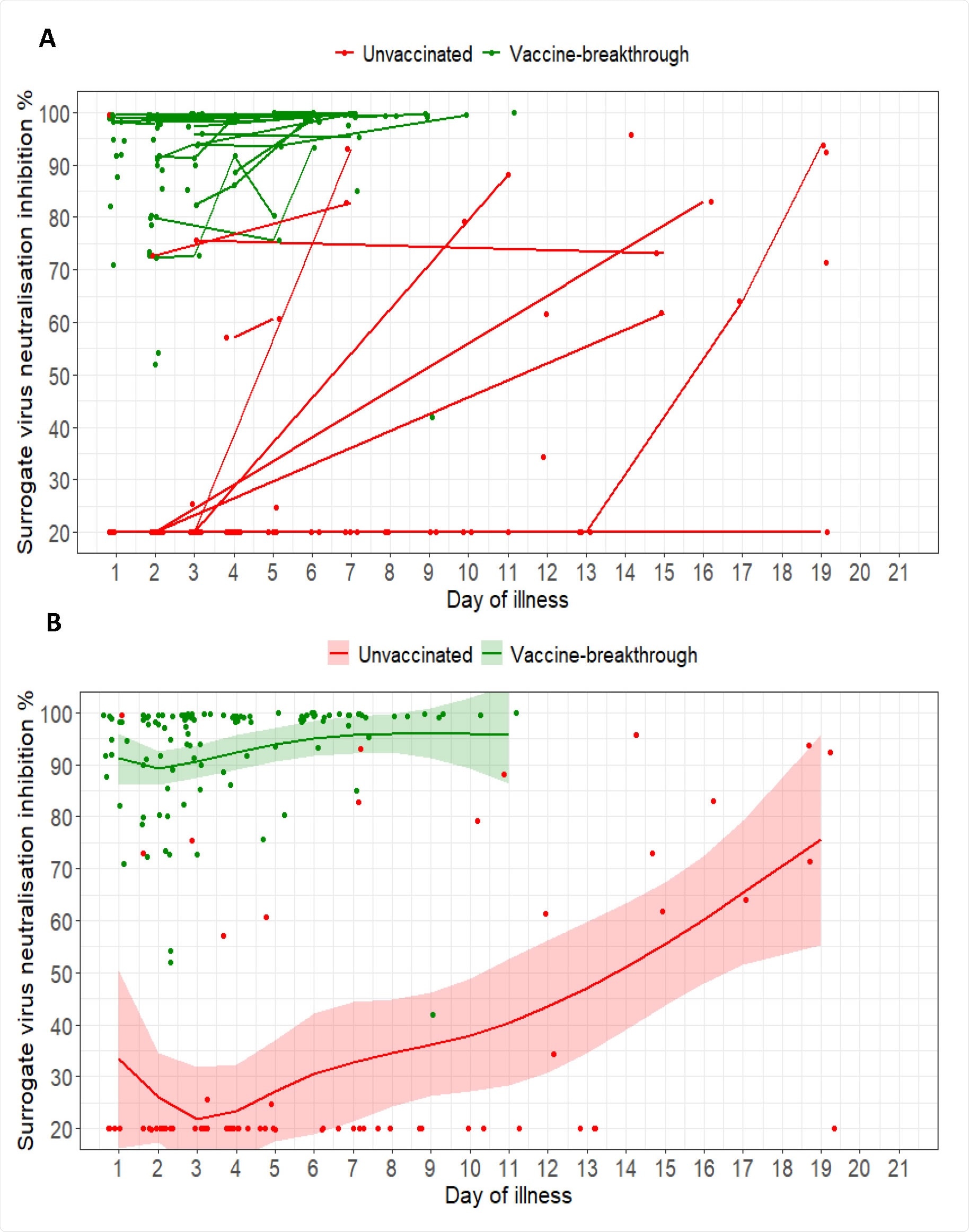
(A) Spaghetti plot of% inhibition of surrogate virus neutralization (sVNT) as measured by cPass; (B) Scatter plot of% sVNT inhibition and marginal effect of disease day by vaccine breakthrough and unvaccinated groups of patients infected with COVID-19 B1.617.2 with 95% confidence intervals from generalized additive mixed models. For the two plots, n = 127; vaccine breakthrough = 67, unvaccinated = 60
Unvaccinated individuals exhibited higher levels of biomarkers known to be associated with more severe disease, including lymphocyte count, C-reactive protein, lactate dehydrogenase, and alanine transferase.
Multivariate logistic regression analysis found that vaccinated individuals were 97% less likely to develop severe COVID-19 requiring oxygen supplementation or moderate illness (defined as the development of pneumonia).
“The finding of a decrease in the severity of B.1.617.2 infection in vaccinated individuals is reassuring and corroborates emerging data from the UK which has shown that mRNA vaccination remains protective against disease. symptomatic and severe, ”the team said.
Learn more about virological kinetics
The initial PCR cycle cutoff (Ct) (number of cycles required for virus detection) values were similar between the vaccinated and unvaccinated groups, at 19.2 versus 18.8.
However, the median value of Ct increased more rapidly over time in vaccinated individuals, indicating a faster decline in viral load.
Researchers say this has policy implications for transmissibility and infection control.
“A shorter duration of infectivity may allow a shorter duration of isolation for vaccinated individuals,” they write.
Learn more about serological results
Of 66 vaccinated people for whom serological data were available, all (100%) had detectable anti-peak antibodies during the first week of illness, compared to seven (16%) of 45 unvaccinated people.
“MRNA vaccines are very effective in preventing symptomatic and severe COVID-19 associated with B.1.617.2 infection,” says Young and colleagues. “Vaccination is associated with a faster drop in viral RNA load and a robust serological response.”
The researchers say that although vaccine infections will continue to be seen, it is likely that there will be a shift to a milder disease spectrum with more widespread implementation of vaccination programs.
“The rapid and widespread implementation of vaccination programs remains a key strategy for controlling the COVID-19 pandemic,” they conclude.
*Important Notice
medRxiv publishes preliminary scientific reports that are not peer reviewed and, therefore, should not be considered conclusive, guide clinical practice / health-related behavior, or treated as established information.


















